Surgical Site Infections
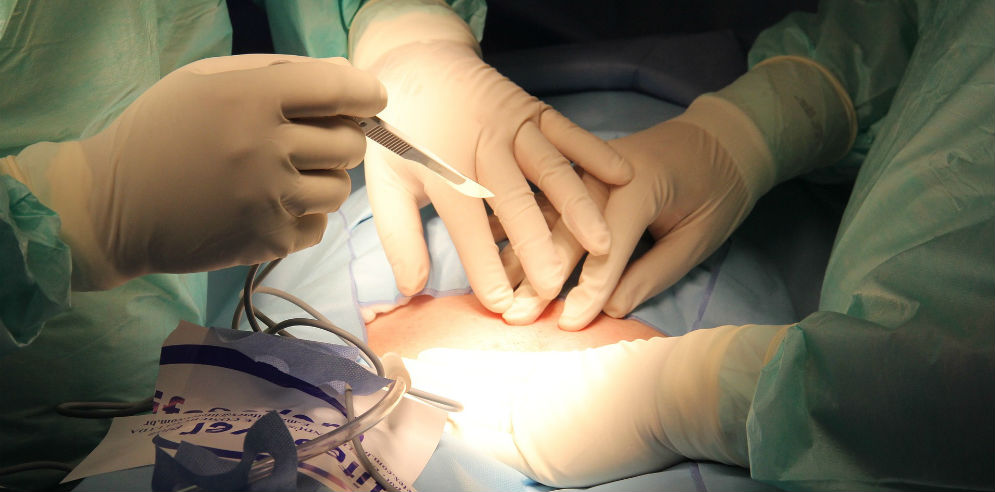
Contaminated hospital operating rooms, equipment or medical staff can lead to serious infections in surgical patients.
Infections that patients suffer from surgical procedures are one type of hospital-acquired infections. Hospital-acquired infections occur frequently, are preventable, and can be lethal. According to the Centers for Disease and Prevention Control, on any day one of every 31 hospital patients has an infection obtained during treatment.
Surgical site infections are the most common hospital-acquired infection, along with infections involving the use of catheters and IVs. All three are caused when the devices or environments are not as clean as they should be.
Symptoms of a Surgical Site Infection
Surgical site infections can develop up to 30 days following a procedure. Signs of a surgical site infection include:
- Tiredness and reduced energy
- Rising fever and chills
- Increasing pain following surgery
- Redness around the incision that lasts and spreads
- Colored, foul-smelling drainage from the incision
A January 2019 article on generalsurgery.com (“Poor Cleaning, High Traffic to Blame for OR Contamination”) reported on research that examined bacteria that cause dangerous hospital-acquired infections. Researchers took over 1,500 swab samples from surgical patients, healthcare providers, surfaces, and surgical equipment – all likely places where dangerous, infectious bacteria live and multiply.
The cultures were labeled “very clean,” “clean,” or “dirty” based on the number of bacteria found.
Going into the testing, researchers expected 90 percent of the cultures to be clean. In reality, less than half (49 percent) of the cultures taken from operating rooms were identified as clean.
Dirty Surgical Equipment
“Never events” refer to preventable medical mistakes that should never happen. Researchers in this study noted two “never events” they found – dirty surgical trays and dirty IV equipment. Contaminated patient IV devices were found in 11 percent of the cultures. Dirty surgical trays were found, too. Following a first surgery, 3.5 percent of the trays were dirty. After cleaning for reuse in another surgery even more surgical trays - 10 percent - were determined to be unclean.
The researchers also tried to determine how the bacteria were introduced into operating rooms, beyond the unclean surgical equipment. They uncovered bacteria transmission trails that were avoidable, such as one instance when a surgical resident brought in bacteria. The bacteria made its way into the anesthesia and then was injected into the IV equipment.
Technology employed in the study produced heat maps that showed where bacteria resided throughout the hospital. Researchers found commonly used rooms that were particularity contaminated with bacteria; dirt that typical cleaning procedures should have wiped out.
Surgical site infections that can turn deadly are not new. Twenty years ago the CDC issued detailed guidelines for preventing surgical site infections. These guidelines offer a blueprint to hospitals for keeping patients, providers, and equipment clean from bacteria that can produce life-threatening infections.
The information covered preoperative issues, such as properly cleaning the patient; operative concerns, such as contaminated surgical attire; and post-op threats, such as incorrect or incomplete patient instructions for proper care of surgical incisions.
The CDC updated these guidelines in 2017.
The threats to patients from surgical site infections are known. The steps to prevent them are also well known. When a life-threatening hospital-acquired infection occurs, there likely was a needless breakdown in care.
If you suffered a serious infection or had a family member die from an infection caused by a mistake in medical care, a medical malpractice attorney will investigate on your behalf.
The choice of a lawyer is an important decision that should not be based solely on advertisements.
Authored by Gray Ritter Graham, posted in Articles March 21, 2019
