Top Medication Errors and How to Prevent Them
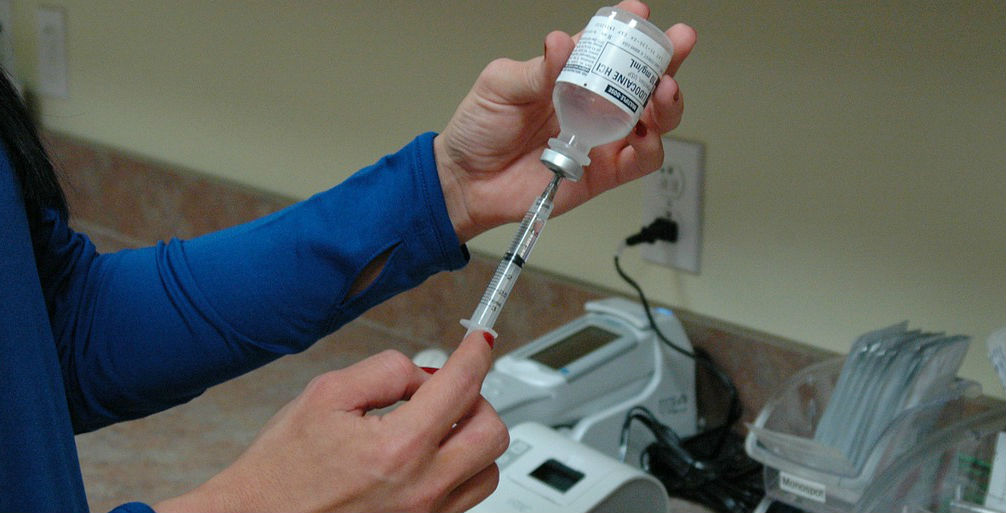
Preventable medical errors have been estimated to be the third leading cause of death in the United States, responsible for the deaths of 250,000 people every year. One of the most common types of medical errors that harm patients is medication errors.
Medication errors include giving the wrong drug to a patient, administering the drug in the wrong dosage, or given the medicine in the incorrect route.
What are the top serious medication errors and what should healthcare professions do to avoid them? A leading safety organization recently provided some answers.
The Institute for Safe Medication Practices is a nonprofit organization that focuses on patient safety, especially with respect to medical drug mistakes that come from administration protocols and unsafe drug labeling and packaging.
Serious Medication Errors are Preventable
At the turn of the New Year, the ISMP published a list of its top 10 reported medication errors from last year. The organization said the errors were not only the most frequent but also posed the most serious harm to patients. And they were also largely preventable by implementing better individual and administrative practices.
First on the list is when healthcare providers select the wrong medication when using computers. This can be done by entering just the first few letters of the desired, appropriate drug. Just like when you search using a specific term and the search engine jumps in before you finish typing with suggestions that aren’t correct, the same can be true with computerized medication technology.
Healthcare professions, the ISMP warns, must be sure to confirm they are choosing the proper drug and not relying solely on computerized results. The organization points out that these technology errors are increasing so fast they now number about the same as mix-ups from handwritten prescriptions.
Communication Problems that Cause Drug Errors
While technology issues account for a growing number of serious medication errors, the ISMP also found problems with person-to-person communication. It cites incidences when spoken given orders are given – either in person or over the phone – in which one person mishears the name of the drug.
Those providing treatment should repeat the name of the drug, even spelling it, to confirm before administering the medication.
Another way the wrong medication may be administered to the patient, according to the ISMP report, is confusion over similar looking labels. Healthcare providers may not pay adequate attention to a drug’s packaging, relying on familiar color schemes and graphics to choose a prescribed drug.
But different drug bottles by the same manufacturers may look alike, or rival manufacturers may have similar label designs. If not vetted closely enough, or when nurses and doctors rely on their preconceived assumptions, the wrong drug may be given to a patient.
Hospitals should store drugs differently or choose different drug manufacturers to avoid such dangerous issues, says the ISMP report.
The ISMP also notes serious problems with providing one anesthetic – tranexamic acid – via the wrong route. It should be given locally but may be administered incorrectly with a spinal injection. Half of the patients die when given this drug with a spinal injection, according the ISMP. Most often healthcare providers confuse other drug packaging with tranexamic acid.
As this reporting of serious medication errors documents, they are highly preventable. When the proper standard of medical care is not provided due to a medical mistake, a patient and the patient’s family can suffer needlessly.
If you had a loved one die or who was gravely injured during medical treatment, an avoidable error may have been made. Speak with an experienced medical malpractice lawyer about investigating further.
The choice of a lawyer is an important decision that should not be based solely on advertisements.
Authored by Gray Ritter Graham, posted in Articles February 4, 2020
