How Miscommunication Can Lead to Serious Medical Errors
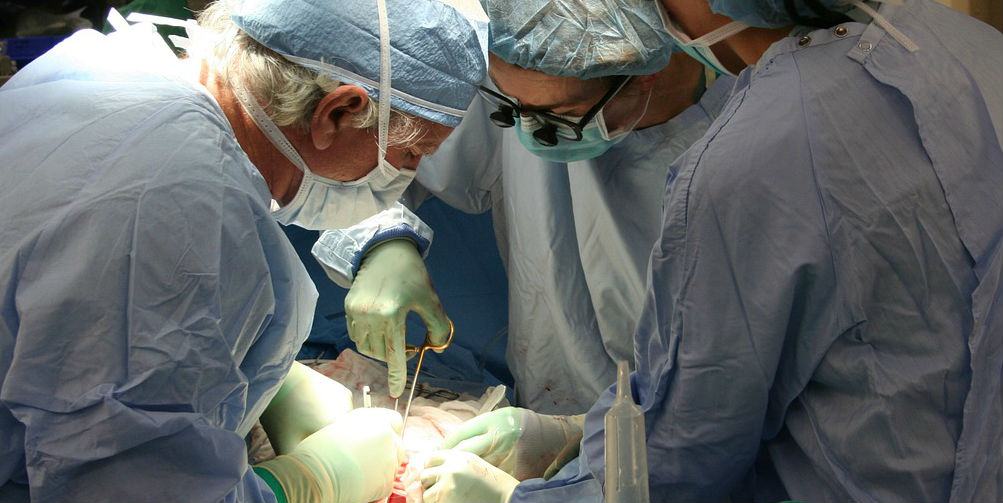
Recent research has shown that unclear communications – even seemingly minor - among healthcare providers can lead to potentially serious surgical errors.
There are many types of commonly made medical errors. Those that pose the most serious health risks for patients include:
- Medication errors
- Diagnostic errors
- Errors in child delivery
- Surgical errors
Preventable Medical Mistakes
Preventable medical errors can forever change the lives of patients and their families. Preventable medical errors are exactly what they sound like: mistakes that shouldn’t have occurred but for some misstep that should have been avoided.
Miscommunication among doctors, nurses and other medical staff is a known cause of serious errors made during medical treatment. Multiple research efforts have shown this cause-and-effect relationship.
The Joint Commission is a leading nonprofit organization that works to improve the safety of healthcare. Accrediting and certifying more than 22,000 U.S. hospitals is one of its roles.
In 2018 it published a whitepaper on communication failures and medical errors, titled “Communicating Clearly and Effectively to Patients: How to Overcome Common Communication Challenges in Health Care.” It identifies several examples of medical communication errors, including:
- Inadequate patient handoffs or transitions of care
- Poor hospital discharge planning and communications with patients
- Errors in test results and medical orders
Errors Made During Patient Handoffs
The Joint Commission preceded that research with a 2012 announcement of a teaching tool designed to avoid miscommunications during patient handoffs. Patient handoffs refer to the period when a new shift of medical staff begins work or when a patient is transferred to different facility.
According to the Joint Commission announcement, 80% of serious medical errors are caused by miscommunication among providers during patient handoffs.
The Institute for Healthcare Communication conducts research and implements educational programs on communication among healthcare providers. It is focused specifically on improving those communications in order to prevent medical errors.
In one whitepaper (“Impact of Communication in Healthcare”), the IHC notes a 10-year study that estimated two-thirds of the medical errors made in that timeframe were caused by miscommunication.
It also notes how communication errors and interruptions during time spent taking patient histories can lead to diagnostic errors.
Ambiguous Communication Can Lead to Surgical Errors
A recent study from the University of Missouri-Kansas City and Kansas University focuses on communication mistakes and misunderstandings that can lead to surgical errors (“Semantically Ambiguous Language in the Teaching Operating Room”).
The researchers – one a linguist - focused on possible misinterpretations between teaching surgeons and their students that ultimately may hurt patients. They did this by studying videos of a small number of surgical procedures done by surgical residents while being supervised.
They found 131 examples of unclear communications between the surgeons that potentially could have harmed patients. This was in just the six videos they reviewed. The study termed these “near misses.” Overall the researchers identified nearly 4,000 examples of potentially ambiguous communications, or about 12 instances per minute.
The researchers contend that any surgical procedure is precise and therefore demands precise communications. Unclear or ambiguous directives are potentially harmful, even if they seem minor. One example provided is a suggestion or question posed by the teaching surgeon that should have been communicated as an order to the resident.
When a patient is seriously harmed during medical care, it can be challenging to determine what went wrong and why. If you lost a loved one and you believe an error in care was made, a medical malpractice attorney can conduct a thorough investigation to determine if a miscommunication or some other preventable mistake was involved.
The choice of a lawyer is an important decision that should not be based solely on advertisements.
Authored by Gray Ritter Graham, posted in Articles August 6, 2021
